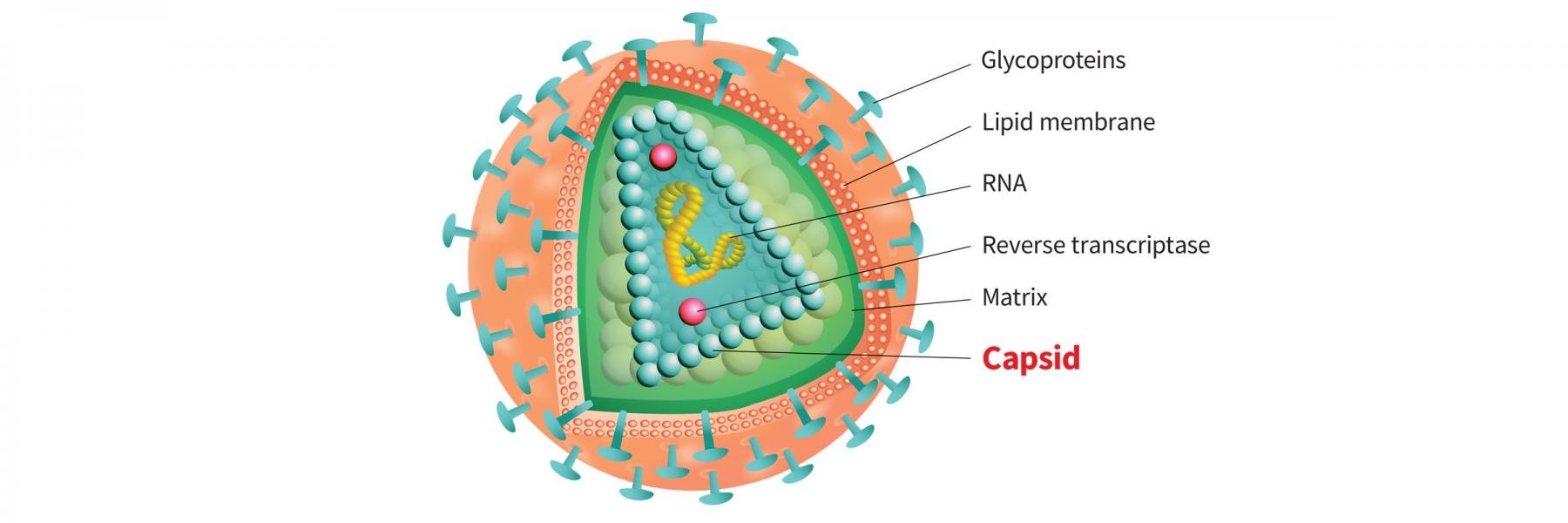
A once-every-six-months formulation of Gilead Sciences’ lenacapavir, the first in its class HIV capsid inhibitor, has been approved by the European Commission, in combination with other antiretroviral medications, for adults with multidrug- resistant HIV who have no other effective treatment options available.
The new regimen requires a lead-in phase with oral lenacapavir tablets, which have also received European approval, before starting the twice-yearly under-the-skin injections. This is not a standalone treatment; twice-yearly lenacapavir still needs to be taken with other HIV medications.
“Lenacapavir provides an innovative long-acting HIV therapy option with the potential to transform the clinical landscape,” said Jean-Michel Molina, MD, Université Paris Cité, professor of infectious diseases and head of the Infectious Diseases Department at the Saint Louis and Lariboi0sière Hospitals.
In the phase 2/3 CAPELLA study, lenacapavir in combination with an optimized background regimen helped 83% of heavily pretreated patients with multidrug resistant HIV achieve undetectable viral load after one year of treatment.
Lenacapavir has no known cross-resistance to other existing HIV drug classes, and has a high barrier to viral drug resistance.
Gilead will market six-month lenacapavir in Europe under the brand name Sunlenca. The commission’s marketing authorization applies to all 27 member states of the European Union, as well as Norway, Iceland, and Liechtenstein.
After resolving a production issue with glass vials, Gilead resubmitted lenacapvir’s application for FDA approval. The FDA has set December 27, 2022 as the target date for its decision. A Phase 3 PURPOSE trial is evaluating lenacapavir as a PrEP drug for preventing HIV.
Read the press announcement here.
—Rick Guasco
Trogarzo wants a faster push
Theratechnologies is seeking FDA approval for a second option for administering Trogarzo. The long-acting entry inhibitor and CD4 post-attachment inhibitor currently has a loading dose of 2,000 mg infused over 30 minutes, with subsequent maintenance doses of 800 mg infused over 15 minutes, The new option would allow for the maintenance dose to be administered as an intravenous push over 30 seconds.
The proposed method would still need to be administered by a qualified health care professional. Administered every two weeks, Trogarzo is for people living with HIV who are heavily-treatment experienced. It must be taken with other HIV medications as part of the regimen.
HIV testing nearly halved during COVID’s first year
The Centers for Disease Control and Prevention (CDC) reported a nearly 50% drop in HIV testing in 2020, the first year of COVID-19, for some populations most affected by the virus. Among tests provided by the CDC in non-health care settings that report race and/or ethnicity data and transmission status, screenings were down from 2019 to 2020 by
- 49% among gay and bisexual men
- 47% among transgender people
- 46% among Hispanic and Latinx people
- 44% among Black people
“HIV testing is the bridge to highly effective treatment and prevention,” the CDC reported in announcing its findings ahead of National HIV Testing Day, June 27. “Delayed diagnoses can lead to negative health consequences and increased HIV transmission.” The agency pointed to its recommendation that everyone between the ages of 13 and 64 get tested at least once and that some people get tested at least annually. To find free and confidential tests, call 1-800-CDC-INFO (232-4636). Rapid tests are also available from pharmacies.
Read the report at bit.ly/HIV-testing-drops-over-covid.
Monkeypox, gay men, and—once again—stigma
With most cases of monkeypox in Europe and the United States occurring among gay and bisexual men, stigma has once again reared its ugly head.
In an editorial, The Lancet Infectious Diseases journal noted, “This raises the question, how to provide health information to a population at risk (here MSM [men who have sex with men]) without stigmatizing them?”
“With outbreaks, such as the current monkeypox one, the most important thing that needs to happen is that those infected seek medical care. Stigma—i.e., blaming and shaming an individual for their infection—can prevent this and, in turn, prevent contact tracing and other containment measures,” the editorial noted. “Some might hope that stigma serves as a corrective of (real or perceived) behavior. However, we know from the ongoing HIV pandemic that shame does not prevent transmission and only leads to individuals suffering and dying in isolation.”
In considering many aspects of information provided, there is also the danger that individuals may become complacent if they feel that the people or groups affected do not include them.
“The messaging is therefore incredibly important. Any message must provide the facts—that certain groups are more at risk and might be more likely to require medical attention—without apportioning blame,” according to the editorial. “It also needs to be accompanied by admissions of uncertainty—e.g., that a certain group is at risk now, but that the virus does not discriminate, and anyone could become infected. This both prevents a false sense of security in the rest of the public and also reduces feelings of frustration or confusion when information is updated.”
The editorial concludes that, “While it may be comforting to believe that a disease can only affect others, such thinking will not control an outbreak and stigmatizing may well extend it.”
Read the editorial, posted July 7 at bit.ly/Lancet-editorial-monkeypox-stigma.
On-demand PrEP? Oui!
Once again (and again), the ANRS PREVENIR Study Group in France reports that on-demand PrEP is just as effective as daily PrEP for preventing HIV among gay and bisexual men: “On-demand PrEP therefore represents a valid alternative to daily PrEP for MSM [men who have sex with men], providing greater choice for HIV prevention.”
During 2017–2019, more than 3,000 participants at 26 sites in Paris were prescribed either a daily pill of Truvada for PrEP or an on-demand schedule of “2-1-1” as used in the IPERGAY study (two pills 2–24 hours before sex, one pill 24 hours after the first dose, and one pill 24 hours after the second dose). About half of the participants elected to use on-demand Truvada for PrEP.
The HIV treatment and prevention guidelines from IAS-USA (the International AIDS Society-USA) recommends on-demand PrEP for MSM.
ANRS is an agency of France’s version of the National Institutes of Health, responsible for funding and coordinating the country’s HIV research. The ANRS study was published in the August 2022 issue of The Lancet HIV.
Students living with HIV awarded scholarships
The HIV League in July announced the award of college scholarships for a cohort of 19 students who are living with HIV. The league is a nonprofit organization dedicated to scholarship, wellness, and education for people living with the virus. Many of them chose to remain anonymous. Among the awardees open about their status are Sabian Castalia, who’s majoring in film production at Brooklyn College, and Martez Smith, a doctoral candidate in nursing and health science at the University of Rochester School of Nursing.
Castalia defines herself as “a queer, Latinx filmmaker and media archivist who strives to use entertainment as a tool to educate and empower audiences.” She began studying film and art as activism in California. She says that her current work “aims to destigmatize sex education and the pursuit of sexual health care by amplifying themes of humor, empathy, and joy.”
Martez holds a bachelor’s of social work from The Ohio State University and a master’s of social work from Long Island University Brooklyn. He is interested in conducting research that “addresses racial, sexual, and gender minority health disparities through community-driven, asset-based interventions.” He also works nationally with activists organizing for social justice with the Keeping Ballroom Community Alive Network (KBCAN), which he co-founded in 2015, and has worked on health and social welfare initiatives. His dissertation explored motivations for sexual health among Black and Latino men who have sex with men in New York City’s house ball community. Martez is a third-time HIV League Scholar. He is also a fellow in the Brown [University] Community and Clinical Research Training (CCRT) Program. CCRT aims to train the next generation of researchers to end the HIV epidemic and to conduct research related to reducing racial disparities in HIV outcomes.
According to the league, this is the only national scholarship program for students with HIV. But, it noted, the scholarships represent more than that.
“Because of the many intersectionalities individuals in the HIV community hold, the HIV League Scholarship also works to bring higher educational equity among LGBTQIA2S+ students, students who identify as a woman, and BIPOC (Black, Indigenous, People of Color) students as well,” the organization reported in its announcement of the awards. This year, the league also set aside monies specifically for a new Trans BIPOC scholarship, for trans-identifying students.
Full-time students are scheduled to receive either $3,500 over one year or $7,000 over two years. Part-time students will receive $1,500 over one year.
Read more about inspirational scholars at hivleague.org.
Bilingual PrEP campaign launches in Chicago
A community-based partnership of HIV service and prevention providers in Chicago has launched PrEPárate, a bilingual campaign in Spanish and English promoting HIV prevention via medicine. One important message: PrEP is free or low-cost for everyone.
The campaign went live in July on the buses and trains of the Chicago Transit Authority (CTA) and on social media (@cookcountyresearch on Instagram). Campaign ambassadors talk about HIV prevention medication in videos posted to preparate.info. ¡Viva!
Prepárate is Spanish for “prepare yourself.” It’s commonly used to say, “Get ready.” It’s the same word used for male and female genders. (In Spanish, some words have a male and a female version.)
Anyone needing help accessing PrEP in Illinois can call the PrEP Hub at (844) 482-4040.
The community partnership was brought together by Cook County Health, Northwestern University, and the University of Chicago. Muy bien, titans. Very good.
PrEP campaign takes to Chicago public transit
Campaña bilingüe para PrEP en Chicago
La campaña bilingüe en inglés y español PrEPárate promueve la PrEP para prevenir el VIH entre las comunidades latinas/x/o en la ciudad de Chicago y todo el estado de Illinois. La PrEP (profilaxis prexposición) son medicamentos que se toman para prevenir contraer el VIH a través de las relaciones sexuales o el consumo de drogas inyectables. La campaña declara que la PrEP es para ti y para mí. Véa videos sobre la PrEP en la página preparate.info. Para más información en español, visite la página preparate.info/español/sobre-la-prep. En Illinois, llame al PrEP Hub para acceder a la PrEP: (844) 482-4040.
From left: Deondre Moore, B. Kaye Hayes, Harold Phillips, Dr. Theresa Tam, and Dr. Howard Njoo following the announcement in Montreal.
U=U gets official backing of U.S. and Canada
In a joint appearance, health officials from the U.S. and Canada announced official support of U=U, Undetectable Equals Untransmittable, at the U=U Global Summit held just before the AIDS 2022 conference in Montreal.
U=U is the science-based principle that a person living with HIV who is on antiretroviral treatment and has an undetectable viral load (less than 200 copies/mL) cannot transmit HIV through sex. The Prevention Access Campaign (PAC) launched the U=U campaign in 2016 to build scientific consensus behind this often-unknown fact.
Harold Phillips, director of the White House Office of National AIDS Policy, made the announcement, accompanied by Kaye Hayes, deputy assistant secretary for Infectious Disease and director of the Office of Infectious Disease and HIV/AIDS Policy at the U.S. Department of Health and Human Services, and Dr. Demetre Daskalakis, director of the Division of HIV Prevention at the Centers for Disease Control and Prevention (CDC).
Calling it a “key message that’s critical to ending HIV,” Phillips shared how U=U counteracted his own internalized stigma. He pledged that the federal government will, “seek opportunities to work with our government and stakeholders to incorporate U=U messaging in federal training, grants, and educational programs.”
Canada’s Chief Public Health Officer, Dr. Theresa Tam, urged all nations to support and leverage U=U to accelerate efforts to end the HIV epidemic.
“U=U is a transformative message for people living with, and affected by, HIV,” Tam said. “It is also an important tool to help us reach our shared targets for diagnosis, treatment and prevention. The evidence behind U=U holds tremendous power to reduce the stigma that can prevent people from getting tested and freely accessing the treatment and support they need.”
Deondre Moore, PAC’s director of U.S. Partnerships and Community Engagement, stressed that addressing health disparities in communities of color is essential to the success of U=U.
“We believe this national and global support is a step in changing that,” Moore said. “We can’t fully celebrate U=U until it is a reality for all, not just the privileged.”
Go to preventionaccess.org for details.
PrEP use data comes to life in new graphics
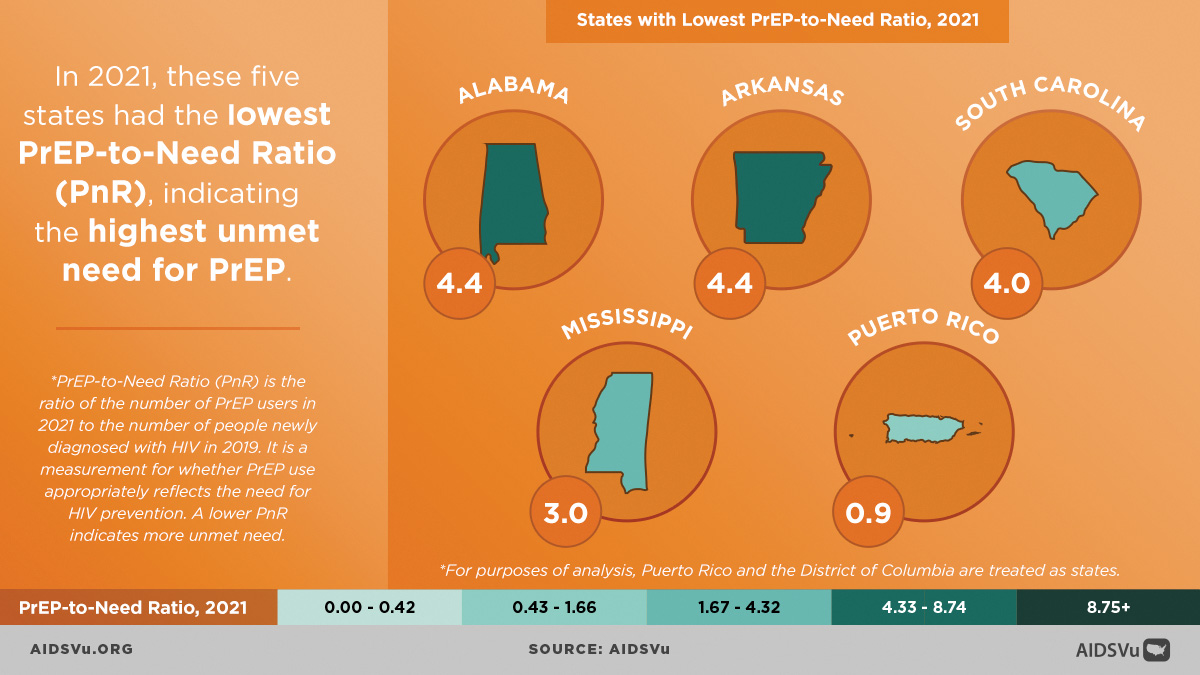
AIDSVu has released a new set of infographics featuring the first-ever publicly available state-level data and regional maps on PrEP use by race and ethnicity, from 2012 to 2021. While use of PrEP has increased an average of 56% each year since its approval in 2012, the graphics depict major inequities in PrEP use among people who are Black and Hispanic, and in the southeastern U.S.
The southeast accounted for 52% of new HIV diagnoses in 2020, yet represented just 39% of PrEP users in the U.S. in 2021. The region also has the states with the highest unmet need for PrEP—Alabama, Arkansas, South Carolina, and Mississippi. (Although Puerto Rico falls under this category of greatest unmet need, it is not a state; it is a U.S. territory.)
“It is important that data do not live in a vacuum and that the insights we glean from research are translated into policy and action,” said Patrick Sullivan, DVM, PhD, professor of epidemiology at Emory University’s Rollins School of Public Health and principal scientist for AIDSVu. “Visualizing PrEP use data on AIDSVu draws attention to underserved people and geographic regions and helps prevention programs better allocate resources to ensure PrEP reaches the people and communities with the greatest unmet need for PrEP.” Dr. Sullivan presented the report on PrEP inequity at this year’s International AIDS Conference (see Happy birthday to PrEP, but not happy equity).
AIDSVu provides interactive maps that visualize the impact of HIV. The site also offers resources to find local services.
Go to aidsvu.org.
—Rick Guasco
Lawsuit charges HIV discrimination at correctional facility
The following story is reprinted with permission from the Good Counsel newsletter of the AIDS Law Project of Pennsylvania, in its Spring 2022 issue. Read the newsletter at bit.ly/AIDS-law-project-fighting-discrimination.
The young man from central Pennsylvania was being held at the George Hill Correctional Facility in Delaware County on a probation violation. He wanted to work in the prison kitchen, but was denied because he is living with HIV.
“John” filed grievances with the privately managed prison, alleging that the staff had discriminated against him because of HIV and had told other inmates about his status. The prison responded that it was simply following policy. He escalated his complaints through the prison’s grievance system all the way to the warden, but at every level his concerns were dismissed.
In the spring of 2020, John contacted the AIDS Law Project of Pennsylvania. Throughout his incarceration, John sent us the denials he received from the facility. He was released in July 2020.
This April, a lawsuit was filed on John’s behalf under the Americans with Disabilities Act in the United States District Court for the Eastern District of Pennsylvania by the AIDS Law Project, Lambda Legal, and Scott Schoettes against Delaware County, GEO Group (the organization that runs the prison), and several individuals. [Editor’s note: Schoettes writes the Poz Advocate column for Positively Aware.]
The complaint alleges violations of multiple laws, including the Americans with Disabilities Act of 1990, the Rehabilitation Act of 1973, and Pennsylvania’s Confidentiality of HIV-Related Information Act.
It’s not the first time that the AIDS Law Project has filed a lawsuit on behalf of a person living with HIV who was denied a job in food services:
As reported in the Fall 2011 issue of Good Counsel, we settled a lawsuit on behalf of a single mother of four living with HIV who was fired from her job at a snack-food factory in Lancaster after her supervisors learned of her status. (bit.ly/Good-Counsel-Fall-2011)
The Spring 2017 issue reported that we reached a settlement on behalf of a chef living with HIV after he and his fiancé were both fired from their jobs at a small-town country club because of HIV. The chef’s fiancé didn’t have HIV, but was fired due to fear of HIV. (bit.ly/Good-Counsel-Spring-2017)
The law on HIV and food handlers is clear. Since 1991, the Centers for Disease Control and Prevention (CDC) has been required to annually publish a list of infectious and communicable diseases that prohibit an individual from working in food services. HIV has never been on the list.
“We believe that this sort of discrimination and carelessness with private information happens all the time in prisons, and largely goes unaddressed,” said senior staff attorney Adrian M. Lowe. “In this case, because of our client’s careful documentation and dogged pursuit of resolution, we had a pile of evidence backing up his allegations.”
The lawsuit demands that the prison develop an anti-discrimination policy and conduct training for all staff regarding HIV, transmission, and universal precautions. The lawsuit also seeks compensatory damages, costs, and attorney fees.