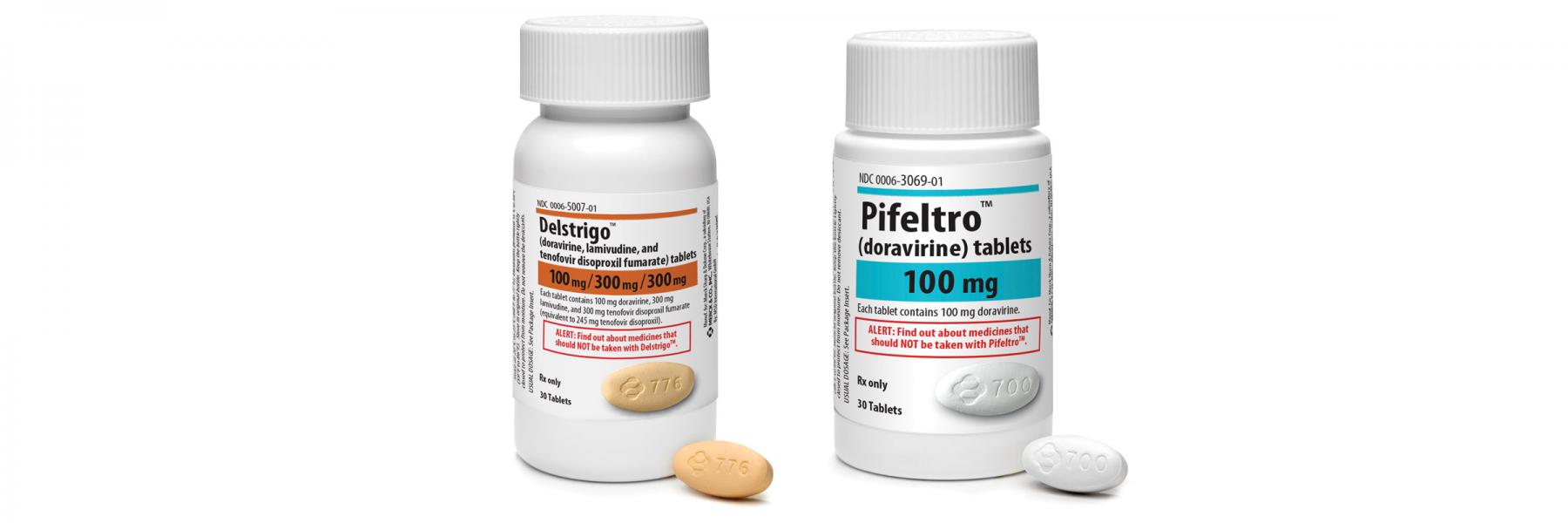
The HIV medication doravirine (DOR) was approved by the FDA in September in two separate formulations. Doravirine is now available as a single-tablet regimen (STR) in combination with 3TC and tenofovir DF, called Delstrigo. A doravirine-only version, available under the brand name Pifeltro, needs to be taken with other HIV medications. Delstrigo and Pifeltro are each taken as one tablet once a day with or without food. The new medications are intended for those who are just starting HIV treatment for the first time (treatment naïve) , but promising Phase 3 switch study results were presented in October (see below). In clinical studies, the most common side effects (in 5% or more of people taking doravirine) were nausea, dizziness, headache, fatigue, diarrhea, abdominal pain, and abnormal dreams. Neuropsychiatric adverse events were reported by 24% of the 324 individuals taking Delstrigo in the DRIVE-AHEAD study. Of these, 12% experienced sleep disorders and disturbances and 9% experienced dizziness. Doravirine is a non-nucleoside reverse transcriptase inhibitor (NNRTI), like efavirenz (Sustiva, found in Atripla). For a review of the new medications, along with their pros and cons, see the inimitable Dr. Paul Sax’s HIV and ID Observations blog (“Doravirine Sets a New Standard for NNRTIs—But What Role in HIV Treatment Today?”) at blogs.jwatch.org/hiv-id-observations.
In the DRIVE-SHIFT switch study presented at IDWeek 2018 in San Francisco, the doravirine STR showed itself to be non-inferior to continuing on a stable HIV regimen.
The 670 participants all started out with undetectable viral load (under 40 copies) for at least six months. None had a history of treatment failure or any drug resistance to the medications in the new STR. For the first 24 weeks, only 447 had been switched to the doravirine tablet from day one (the immediate switch group). At 24 weeks, the remaining 223 participants were also switched (the delayed switch group). At the end of 48 weeks, more than 90% of each group maintained their undetectable viral load (less than 50 copies).
Search for the abstract online, “Switch to Doravirine/Lamivudine/Tenofovir Disoproxil Fumarate (DOR/3TC/TDF) Maintains Virologic Suppression Through 48 Weeks: Results of the DRIVE-SHIFT Trial (LB2).”
The hepatitis C (HCV) medications Harvoni and Epclusa are coming out as generics. Gilead Sciences, Inc., manufacturer of both drugs, announced in September the creation of a subsidiary company to produce the generics. “We believe that introducing these authorized generics is the fastest way to lower list prices for our HCV cures without significant disruption to the healthcare system and our business, as a bridge to longer term solutions aimed at reducing patients’ out-of-pocket medication costs,” according to a Gilead press release. “Starting in January, health insurers will have the choice of covering our branded medications or the authorized generics.” The new subsidiary is Asegua Therapeutics. The list price for the new generics is $24,000 for the most common course of treatment (8–12 weeks for Harvoni and 12 weeks for Epclusa). Harvoni is the brand name for the combination of ledipasvir and sofosbuvir; Epclusa is the brand name for the combination of sofosbuvir and velpatasvir.
People living with HIV who inject drugs cut their risk of death in half with a counseling and treatment support intervention, according to an international study. A press release from NIH says, “They also were about twice as likely to have suppressed their HIV to undetectable levels after one year. The intervention consisted of psychosocial counseling along with guidance and support navigating the healthcare system.”
“People living with HIV who inject drugs often encounter multiple obstacles to beginning and adhering to treatment for HIV infection and substance use,” said Anthony S. Fauci, MD, director of the National Institute of Allergy and Infectious Diseases (NIAID), in the release. “This study demonstrates that providing guidance and counseling can help such individuals overcome barriers to starting and staying in care and treatment, leading to a significantly higher rate of HIV suppression and a much lower rate of death.”
In the intervention, a systems navigator helped individuals overcome such barriers as not knowing how to enroll in HIV medical care or trouble keeping appointments. Psychosocial counselors helped them overcome psychological obstacles they may have to starting and staying in treatment, such as lack of interest in therapy, stigma, or trouble with maintaining a medication routine.
“People who inject drugs and are living with HIV have potentially fatal co-occurring conditions, yet they and their at-risk partners often face different and confusing care delivery systems,” said Nora D. Volkow, MD, in the release. She is director of the National Institute on Drug Abuse (NIDA), which co-funded the study with NIAID. “This study shows that integrated interventions, including help from systems navigators, can dramatically reduce mortality for both conditions.”
HPTN 074 enrolled 502 men and women living with HIV from Indonesia, Ukraine, and Vietnam, along with 806 of their injection partners. The study was published September 1 in The Lancet.
“Many transgender youth lack access to transgender affirming care, which may put them at risk for HIV,” reported Celia B. Fisher, PhD, director of Fordham University’s Center of Ethics and Education, and colleagues in the August 2 issue of the journal LGBT Health. An internet survey of 228 trans youth ages 14–21 found that half had not disclosed their gender and sexual minority (GSM) identity to a primary care provider (PCP) due to concerns about a lack of acceptance. One-quarter did not disclose due to concerns that their parents would be notified. Another 25%, however, felt that their provider was helpful with GSM sexual health issues. “Transgender youth may not discuss their GSM identity or sexual health with PCPs because they anticipate GSM stigma and fear being ‘outed’ to parents,” the researchers concluded. “PCPs should receive transgender-inclusive training to adequately address youths’ sexual health needs and privacy concerns.”
The American Academy of Pediatrics (AAP) in September issued its first policy statement on transgender children. “Despite increasing public awareness and some legal protections, children who identify as lesbian, gay, bisexual, transgender, or gender-diverse often lack adequate health care, including access to mental health resources,” the academy said in a press release. The policy statement “reviews the latest research and provides recommendations that focus specifically on children who identify as transgender or gender-diverse, a term used to describe people with gender behaviors, appearances, or identities that do not align with those culturally assigned to their birth sex.” The academy noted that its underlying theme is that, “Transgender and gender-diverse children face many challenges in life, but, like all children, they can grow into happy and healthy adults when supported and loved throughout their development.” Read the press release and the statement, published online September 17, at aap.org. According to its website, the AAP represents 67,000 pediatricians in the U.S.
“Ending HIV is Everyone’s Job,” the New York-based Latino Commission on AIDS declared for National Latinx AIDS Awareness Day, October 15. The commission said the theme focuses on the tools currently available to address HIV: “take the HIV test; consider PrEP as a prevention approach; stay adherent to HIV treatment to become virally suppressed or undetectable; and use condoms.”
“New HIV diagnoses among Hispanics/Latinx have increased while the incidence of new diagnoses have decreased or remained stable in the other ethnic groups,” the organization reported in a press release. “We see the impact of stigma, homophobia, and transphobia in accessing HIV testing, prevention, treatment, and care in our community.”
For more information: cdc.gov/hiv/group/racialethnic/hispaniclatinos/index.html
Erradicar el VIH
“Erradicar el VIH” fue la declaración the Latino Commission on AIDS para el Día Nacional Latino para la Concientización del SIDA, el 15 de octubre. La organización notó que la tema enfoca en las herramientas disponible para trabajar con el VIH: “hacerse la prueba del VIH, considerar PrEP como un método de prevención, mantenerse recibiendo tratamiento de VIH para alcanzar la supresión viral y permanecer indetectable, así como usar condones.”
“Los casos nuevos de VIH han aumentado entre los Hispanos/Latinx mientras que la incidencia de nuevos casos diminuyó o permaneció estable en los otros grupos étnicos. Podemos ver así el impacto que el estigma, la homofobia y la transfobia tienen en la formación de barreras para el acceso hacia la prevención, tratamiento y cuidados del VIH, así como también sobre el acceso a pruebas de detección de VIH, prevención, tratamiento y cuidado medico en nuestra comunidad,” la comisión notó en un comunicado de prensa.
Para más información en español:
cdc.gov/spanish/especialesCDC/VIHDiaLatino
LGBTQ activist and drag performer Zak Kostopoulos, 33, died in Athens on September 21 after a beating captured on video. According to a report from NBC News, the attackers claimed Kostopoulos was trying to rob their store while his friends say he was seeking shelter from a brawl outside. Kostopoulos raised HIV awareness through the organization Positive Voice. More than 500 people attended a rally in his honor the day after he died.
Zak Kostopoulos
Last year, on September 28, Bernard J. Brommel, PhD—Bernie to his friends—attended TPAN’s 30th anniversary celebration, receiving an award for “A Legacy of Devotion” along with other founding members of the organization, including other long-term survivors of HIV like himself.
In 1987, TPAN founder Chris Clason had made a call out to Chicago for help in building TPA (as it was then called) and Bernie was one of those who answered the call. He served on the first board of directors and performed any number of services. There were no staff members then, so volunteers helped TPAN run as smoothly as possible, and assisted members in obtaining the information and support that they so desperately needed. At one point Bernie led a campaign to have memorial gifts made to TPA, especially after seeing the property of members go to families that had disowned them. He was then in his 50s, and survived to see the 30th anniversary of the organization he, along with others, helped build.
This year, on September 22, Bernie passed away at the age of 88, having entered hospice care a week earlier, after years of heart disease and regular kidney dialysis. “His final hours were peaceful,” baritone and music professor Carl Ratner, Bernie’s partner of more than 20 years, wrote in his announcement. Thanks to safer sex and U=U, Carl has remained HIV negative. Empowering people in their treatment decisions has been but one aspect of TPAN’s work.
Bernie was a professor emeritus of Northeastern Illinois University, in Chicago, where he taught for 28 years, in the Department of Speech and Performing Arts (now the Department of Communication, Media and Theatre). There he was also a leader in many university functions. He was also a family therapist. He became the university’s first million-dollar donor, eventually donating a total of $2.5 million. In a tribute from the school, Northeastern noted that it had in 2010 renamed the science building the Bernard J. Brommel Hall in honor of his support over the years, which included the establishment of 25 scholarships.
Gifts often keep on giving. Not five years ago, one of those scholarships went to a young gay man studying social work who was placed, coincidentally, at TPAN for his internship. That young man met Bernie at a school social function for the awardees, where he then heard stories about the early days of TPAN. Bernie was forever proud of Northeastern and helping students. He had asked that the school’s pennants and his cap and gown be placed on his casket.
Bernie grew up in poverty on an Iowa farm, milking cows before going to school. It was a hard life, with a difficult father, and it was also homophobic. He said he didn’t know the meaning of the word “gay” when he first heard it. He entered a long-term marriage and had six children before divorcing and becoming his true self. It wasn’t until after his mother died that he came out as a gay man.
He never stopped working to help others, even continuing to write and publish in his final years. Wrote longtime HIV activist Lori Cannon, founder of Open Hand Chicago (now Vital Bridges), then the only food pantry for people living with HIV, “RIP, Bernie. You done good.”
Rest in power as well.
This year, TPAN’s Ride for AIDS Chicago (RFAC) recognized 15 years of community engagement and fundraising to support the life-saving services of TPAN and Positively Aware. Over the weekend of September 7–8, more than 200 volunteer cyclists, crew, and supporters covered more than 200 miles in two days. Their stories reflect the many reasons and ways in which we all advocate for people living with and affected by HIV.
This year, two father-son teams inspired us all with their love for each other and their dedication to TPAN’s mission.
Dr. John Schneider, an HIV researcher and specialist in Chicago, rode the 200 miles with his 12-year-old son, Mahin, who was the youngest-ever participant in the Ride’s 15-year history. They both were quickly embraced and supported by all the cyclists and volunteers. As he told Windy City Times, “I work in HIV and know firsthand what people living with HIV go through as well as those who are vulnerable to HIV. The outpouring of support for Mahin was incredible and not what I had expected.
Steven Acosta (above, right) had participated in RFAC previously, and this year he and his father Orlando rode as a team. Steven shared his experience this summer with GoPride.com, saying, “There is someone close to me who died of AIDS many years ago…I ride for the community…. Doing 230 miles with my dad [is] an experience I will cherish my whole life.
Each year around September 21 (coinciding with the autumnal equinox) for A Day with HIV, some entries are prosaic, others poignant. This year, we wanted to give space to an entry for which there is not enough room in the ADWH pages, for the story it tells about treatment and resilience. See more photos from the 2018 A Day with HIV at adaywithhiv.com.
10:17 AM: Portland, Oregon
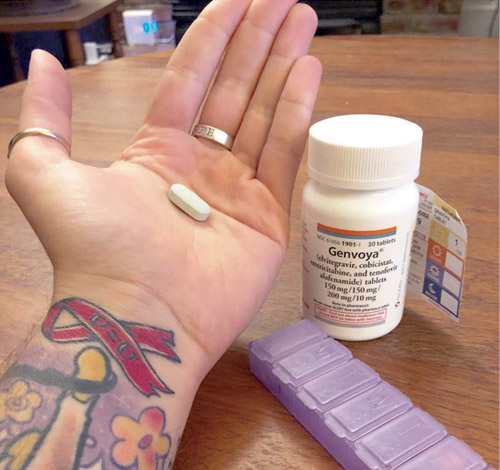
Anthony: When I first found out I was HIV positive I thought it would define me—but by “define,” I came to realize I really meant “stigmatize.” I felt like there would never be a part of me inseparable or irreducible from the virus itself. The thought of having it constantly preoccupied me. Each day when I swallowed that little greenish pill in the morning, I felt a pang of shame and sadness. Today, after living healthily with HIV for three years, the greenish pill still punctuates my days, but the feeling is one of propulsion and determination in place of despair, guilt, and self-loathing. How far I’ve come!
I happened to have an appointment scheduled with my HIV specialist at Prism Health today, so I took the opportunity to snap a selfie in celebration of taking control of my sexual health.
Speaking of health, specifically the medication and insurance end of it, I’ve attached an image of the receipt for the pill that I need once daily to stay alive.
The retail cost of a 30-day supply of these pills is $3,467.99. For those like me who don’t excel in arithmetic, that is approximately $116 per day. It feels funny taking something that expensive every day, but I thank my lucky stars that my insurance completely covers this cost. There are also last-resort secondary insurance non-profits for people with HIV that exist to pick up the excess cost should one’s insurance not cover it.
The precariousness of our government and the current administration means that some of this funding for HIV/AIDS research and for these non-profits is in jeopardy of disappearing. What would a person like me do then? I’m glad that is not our current reality. Anyway, fuck stigma and live your best life! Like my tattoo reminds me, I am still me.
What used to be called “female condoms” have been reclassified by the FDA as “internal condoms.” According to the National Female Condom Coalition (NFCC), there are three important changes. The sexual health device is now:
- “Renamed as a ‘single-use internal condom,’ a change that de-genders the prevention tool and provides a more inclusive description of who is encouraged to use and benefit from it.
- “Transitioned from the regulatory Class III to a Class II, a move that will lessen the burden on manufacturers when seeking FDA approval for existing and newly developing versions of internal condoms.
- “Approved for both vaginal and anal intercourse, thus endorsing use of this tool for a wider spectrum of sexual activities.”
According to Sara Semelka of the AIDS Foundation of Chicago, which serves as the NFCC Secretariat, “We are thrilled to learn about these changes and so grateful for the tireless efforts of sexual health advocates across the globe who worked for years to demand greater access to this prevention method, which truly empowers people to take control of their health on their own terms.”
The condom reclassification was announced in September.