“If we are really serious about retention in care for women living with HIV, we have to do the underlying work. You are bringing everything with you to the clinic, not just HIV.”
—Vanessa Johnson,
co-owner, Ribbon Consulting Group;
Co-founder, Positive Women’s Network-USA;
founder, Common Threads
Women living with HIV experience multiple barriers to HIV care—both accessing care and experiencing the full benefits of care once connected.
Decades of research and clinical experience both within and outside the HIV community have shown a stark link, across races, ethnicities, genders, and socioeconomic backgrounds, between past and recent trauma and a wide range of chronic conditions and poor health outcomes. These statistics are especially troubling among people of color, particularly African Americans.
Successful treatment for chronic health conditions such as diabetes, depression, obesity, heart, lung, and liver diseases, substance use, and sexually transmitted infections including HIV, is often disturbingly elusive—in part because clinicians and care environments fail to address the trauma and post-traumatic stress disorder (PTSD) that underpin them.
A parallel body of evidence shows the overwhelmingly high burden of violence (including institutional violence, racism, and other forms of systemic injustice), abuse, and PTSD among women living with HIV—about 80 percent of whom are women of color, and most of whom are living in poverty—including the reality that three in four women living with HIV report a history of gender-based violence.
Meanwhile, there is a crater in the HIV care continuum for women living with HIV, by last gender-stratified count: 70 percent of women connect to care, but fewer than half of them remain in care.
Transgender women, historically, have some of the worst HIV health outcomes by many measures: very low rates of engagement and retention in care, high rates of loss to follow up, and in some studies, lower rates of HIV medication use than among injection drug users. The HIV rate among transgender women is disproportionately high: 2.6 percent among transgender people as a whole, and up to 4.4 percent for African American transgender women.
What’s the connection between trauma and barriers to care for women living with HIV?
Women may have specific experiences, compounded by gender, that create unique barriers to their accessing HIV care. Wraparound services like peer-based, gender-responsive programming; transportation, housing and childcare assistance; nutritional support; and mental health and substance use treatment are essential for many women to be able to receive consistent and high-quality care. If these services are absent, a woman’s ability to stay connected to HIV care becomes even more tenuous.
But even in a landscape of supportive services, trauma and violence continue to erode the health outcomes of women living with HIV in what Positive Women’s Network-USA (PWN-USA), a national membership body representing women with HIV, has called a “crisis of unaddressed trauma among women living with HIV”—which may be the missing ingredient to account for systemic failure to provide high-quality care for women with HIV.
If the National HIV/AIDS Strategy is to reach the stated commitment of its second goal—increasing access to care and improving health outcomes for people living with HIV, and to meet the challenges therein—providers must be supported in their efforts to think and practice outside the box, to adapt innovative models to meet the needs of women living with HIV in their communities.
Medical University of South Carolina Ryan White HIV/AIDS Clinic:
Struggling to keep women connected to care in South Carolina
Part D of the Ryan White HIV/AIDS Program serves women, young people, and families living with HIV in the U.S., and contributes to Ryan White’s relative success retaining women with HIV in care—in part due to the essential wraparound services Part D
is able to fund.
The Medical University of South Carolina (MUSC)’s Ryan White HIV/AIDS Clinic is funded in part through Part D. According to Lauren Richey, MD, of MUSC, in addition to medical care, MUSC provides transportation assistance, social work services including counseling, dental care, medication assistance, case management, peer navigation, housing assistance, nutritional supplements, meal tickets, substance use treatment referrals, and emergency financial assistance. They also have a new, on-site psychiatry clinic, where clients can be seen, evaluated, and followed by a psychiatrist in the same clinic space; and a women’s health clinic where sexual and reproductive health care are available to women with HIV at all parts of their lifespan, from PrEP and preconception counseling to post-menopausal care.
Last year, when MUSC staff identified roughly 19 percent of their clients that they defined as “not retained” in care (meaning they didn’t meet MUSC’s criteria of having had two visits separated by 90 days over a one-year period), they set out to find out what had happened to them, and to get them back into care. Fifty-five percent of those folks were discovered to have “fallen out of care” (others’ absence was found to be due to transferring care, experiencing incarceration, or passing away). Those who “fell out of care” were more likely to be female, African American, and have lower CD4 counts and higher viral loads than those who transferred care.
“Linda [the clinic’s licensed professional counselor] completed a step-wise series of outreach: phone, letter and home visits to try to reach and re-engage our patients who are lost to care,” Dr. Richey explains—and that intervention has been effective in getting clients to come back for a visit. But barriers remain to reaching clients who may need interventions like substance use treatment the most.
Even this level of care is unheard of for most health conditions—and is sorely needed in order for tens of thousands of people living with HIV to remain connected to care. But a growing number of providers are taking yet another innovative step to increase the effectiveness of the care they provide—and their clients’ capacity to access it.
The Ryan White HIV/AIDS Program’s models of care made it a pioneer in community-responsive health services. Recently, advocates have called for trauma-informed approaches to be the next legacy of the Ryan White HIV/AIDS Program—to solidify a bold standard in HIV care prioritizing environments that contribute to healing.
Christie’s Place staff and clients. Photo: Louis “Kengi” Carr
‘All of our staff—those who do administration, bookkeeping, outreach—everybody had to become competent, aware, and savvy about the principles and practices of trauma-informed service provision.’
—Erin Falvey, Executive director, Christie’s Place
Christie’s Place:
Building foundations for a trauma-Informed environment for women in San Diego
“I think it’s just the empathy that is exhibited here,” says Jay Blount of what sets Christie’s Place, a support services center for women, children, and families impacted by HIV in San Diego, apart from other area providers. “Clients love it because it’s a home-like environment; it’s not all about HIV.”
Blount is a family case worker at Christie’s Place, as well as a peer navigator through its CHANGE (Coordinated HIV Assistance and Navigation for Growth and Empowerment) for Women program, helping women living with HIV like herself to engage with and stay in care. Christie’s Place is literally based in a house, in a residential neighborhood. “Women can come and relax, get on the computer, just hang out, cook if they need to,” says Blount. “It’s not appointment based; we interact with clients all day long. Other places are very clinical, sterile.”
And as the staff at Christie’s Place is well aware, for women with trauma histories, a clinical medical environment can be re-traumatizing and become, in itself, a barrier to accessing care.
“One of the hallmarks of a PTSD diagnosis is avoidance of reminders of a traumatic event,” Erin Falvey, Christie’s Place’s clinical director, explains. A medical or social-service environment can be a reminder of traumatic events for myriad potential reasons: invasiveness of procedures; unanticipated shifts in providers that can assault an already fragile sense of trust; or, for those who have experienced male violence, a clinic waiting room that may often be filled with men.
Falvey and Blount were both part of Christie’s Place’s process of becoming a fully actualized trauma-informed agency. The Substance Abuse and Mental Health Services Administration (SAMHSA) promotes a trauma-informed approach that shifts from the traditional medical view of “What’s wrong with this person?” to a more holistic framing—“What happened to this person?”—as a foundation for healing and recovery. According to SAMHSA, a trauma-informed environment
- realizes the widespread impact of trauma on the population;
- recognizes the signs and symptoms of trauma in clients, families, staff, and others involved with the system;
- responds with full integration of trauma knowledge into policies, procedures, and practices; and
- resists re-traumatization in the care setting.
(Read more about SAMHSA’s principles of a trauma-informed approach: samhsa.gov/trauma-violence/samhsas-efforts.)
“Recognizing trauma is likely part of the client’s history, that may be playing out in how she’s showing up, helps us to see her resiliency—and to have a different level of compassion in our work,” Falvey says.
The year 2012 saw the publication of two key studies led by Edward Machtinger, MD, director of the Women’s HIV Program (WHP) at the University of California, San Francisco (UCSF): one showing, for the first time, a significant link between recent trauma and HIV-related health challenges for women living with HIV; the other a review of 29 studies revealing that women with HIV were two to six times more likely to have experienced traumatic events and PTSD than women in the general population—and that 60 percent of women with HIV reported lifetime sexual abuse, more than 5 times the percentage among women who reported the same in a general sample of women. (Read an interview with Dr. Machtinger at thebodypro.com/content/74768/unraveling-the-impact-of-trauma-on-people-with-hiv.html.)
This was around the time Falvey arrived at Christie’s Place. A licensed marriage and family therapist, she brought with her a history of working with trauma, and saw an immediate need for Christie’s Place to become more trauma focused. “[Dr. Machtinger’s research] really helped us to substantiate the data backing the link between trauma, PTSD, and women’s health outcomes,” Falvey says. Machtinger has since teamed with UCSF providers, in partnership with PWN-USA, to develop and publish an adaptable model for trauma-informed primary care. (Get more practical information about this trauma-informed care model: whijournal.com/article/S1049-3867(15)00033-X/fulltext.)
The CHANGE for Women program already worked to deliver crucial support services that address women’s barriers to staying in care, in a safe space. In addition to counseling and outreach, Christie’s Place supports women who may be balancing multiple, competing survival priorities. The agency provides assistance to meet basic needs—hygiene products and food, baby diapers and formula—as well as onsite childcare and transportation support, a resource whose value cannot be overestimated in sprawling San Diego County, where travel for a clinic visit can run up to three hours one way. Christie’s Place also partners with a local public-interest law firm that can help with immigration relief—of tremendous concern to many clients in this border city—and employs many bilingual staff members, to make all Christie’s Place services available in English and Spanish. Since Christie’s Place implemented CHANGE for Women, women’s engagement in HIV care in San Diego County has increased by 14 percent.
“We were actually doing [trauma-informed] work already,” Blount says. “Now we have the language to go with it—we know what it is.” Equipped with a Retention in Care grant from AIDS United and the MAC AIDS Fund, Christie’s Place solidified its foundation as a trauma-informed agency. “All of our staff—those who do administration, bookkeeping, outreach—everybody had to become competent, aware, and savvy about the principles and practices of trauma-informed service provision,” Falvey says.
The staff is predominantly female—of 18 current members of the team, two are men. Statistics of violence experienced among women in the general population already suggested a high likelihood that Christie’s Place staff would have gone through similar experiences to the ones they learned about through the Office on Women’s Health (OWH)’s trauma-informed trainings. “And we saw that,” says Falvey, “really, really quickly.”
Peer counselors in trauma work are considered “two-hatters,” wearing the “hats” of trauma survivors as well as service providers. “Our peer navigators are three-, four-, and five-hatters”—often bringing a combination of substance use and violence histories and mental health diagnoses, in addition to living with HIV and surviving trauma. Many of the staff who were not living with HIV also had violence histories.
Built into Christie’s Place’s model are strong commitments to supervision and peer support, as well as self-care, for all staff, supported by policies and practices like a wellness committee and time off for staff members’ own therapy appointments. Though it can bring up painful experiences, Falvey believes the trauma-informed training and commitment help staff to feel far more prepared—and to see their own resiliency as well as that of their clients.
A key tenet of OWH’s and SAMHSA’s trauma-informed principles is that healing happens in relationships. “One of the most powerful things we can do is recognize that we all have the ability to help facilitate trauma recovery by how we are in relationship with people that we serve,” Falvey concludes. “Everybody has that potential, not just providers. It’s all about the relationships and the environment that you’re facilitating.”
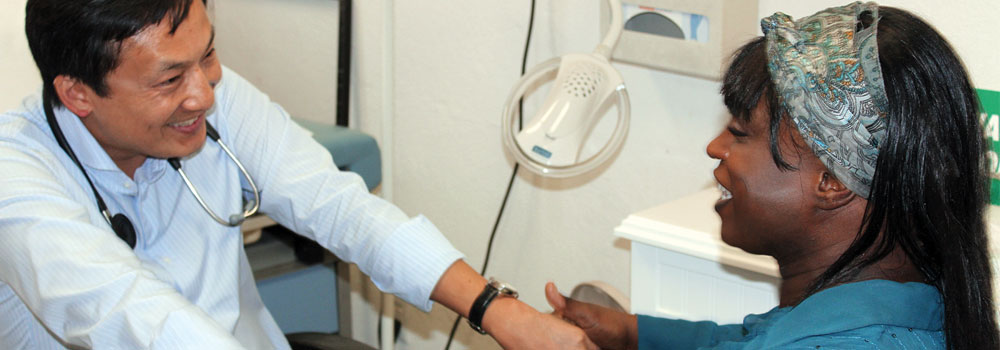
Dr. Lin with Johanna Brown, a client in API Wellness Center’s TransAccess program.
(Photo Courtesy of Asian & Pacific Islander Wellness Center.)
‘For folks who are the most vulnerable and the most in need, conventional medical structures oftentimes aren’t able to meet the level of need.’
—Royce Lin, MD, San Francisco department of public health
TransAccess:
Connecting women to care in the midst of complex lives
“I think we’ve been setting people up to fail,” states Royce Lin, MD, of conventional medical models of health care. “The more intersections of disparities that populations face, the higher a level of care is required to address them.”
Dr. Lin’s main job is at the Tom Waddell Urban Health Clinic—among the first publicly-funded clinics providing services and care specifically for transgender clients, which recently celebrated its 25th anniversary in the Tenderloin community of San Francisco. There, the environment is more of a traditional, large clinic. But for the past several years, thanks to a grant from the Health Resources and Services Administration (HRSA)’s Special Projects of National Significance (SPNS), Dr. Lin has been able to bring trauma-informed principles to bear in serving clients with extraordinarily chaotic lives.
The demonstration project, called TransAccess, endeavors to improve access and retention to care, and often abysmal health outcomes, for transgender women of color living with HIV. “The clients we work with have not done well within existing conventional systems of care,” says Lin. Of about 50 patients who have received primary care through the program, about one-third started the program with advanced HIV, 80 percent or more are homeless at time of entry, and about 70 percent have serious mental health challenges including psychosis, often related to meth use as a coping mechanism for survival on the streets. Many women rely on survival sex work to get by.
“For folks who are the most vulnerable and the most in need, conventional medical structures oftentimes aren’t able to meet the level of need,” Lin says.
National data reflect that all manner of social structures have historically done a terrible job meeting the needs of transgender women—particularly looking at the intersectionality of the incredibly high preponderance of poverty and trauma in the population, and coping mechanisms to trauma that cause more harm. High rates of family rejection, employment discrimination and limited educational opportunities, all underpinned by systemic bias, combine to create dire survival circumstances, and correlated HIV vulnerability, for many transgender women of color.
Further, a recent Transgender Law Center survey found that 48 percent of transgender respondents feel it is reasonable to avoid treatment. “It’s not that trans people don’t care about their health,” says Lin. “Those who stay away from care do so because of experiences they’ve had”—including a high likelihood of past negative experiences in a health care setting.
For example, for transgender individuals, being misgendered by clinic staff can be not only personally distressing, but physically unsafe. “Calling out ‘Mr. Jones’ in a crowded waiting room, and the person who stands up is feminine in her presentation: Right then she has been outed—and may be victimized or targeted for violence when walking out of the clinic,” Lin explains. “There may be no malice behind it from the staff, but the result is still that it ruins a client’s whole day”—and makes it less likely for the client to return.
These concerns in health care settings can be addressed with greater transgender sensitivity and cultural competency, appropriate training and tweaks to the clinic environment to signal a culture of welcome and safety for trans people living with HIV. Posters and visual cues featuring trans subjects, as well as gender-neutral bathrooms, are a good start. Transgender professional organizations also recommend that medical forms adopt the “two-step ask” regarding gender—”What is the gender you were assigned at birth?” and “What gender do you identify as currently?”—to combat harmful misgendering experiences.
The TransAccess program is not based at the main, large, more anonymous clinic. Instead, for that half-day per week, the medical team is out-based at the Asian-Pacific Islander Wellness Center (API Wellness)—home of TRANS:THRIVE, the largest trans drop-in space in San Francisco, and a longtime HIV service organization in the Tenderloin.
“Right off the elevator, the vibe is different,” explains Lin; like Christie’s Place, it is less institutional, cozier. “Thursday is clinic day, and folks just show up.” Transgender staff and peers are highly visible; the clinic staff is small, and can be easily accessed outside clinic hours. An open-access model of care counters the difficulty of keeping strict appointments amidst complicated priorities. The space provides opportunities for building community and leaving behind the competitive nature of life on the streets. A wellness group, run by two trans women of color, focuses on topics like gender affirmation (social interaction that affirms one’s gender expression—often elusive for trans women, whose gender expression is often not affirmed but defamed), gender empowerment, and finding voice.
“For many clients, HIV is about number nine on their list of priorities,” says Lin. For instance, a caring provider typically worries if a patient has a low CD4 count, and may want them to start HIV meds above all else. “That is the provider’s priority.” The client’s priority may be finding a place to sleep, dealing with a violent john, or accessing hormone therapy, and may feel pushed to get their HIV under control when other aspects of their life demand their energy. “At best, the approach doesn’t resonate; at worst, it comes across as insensitive and out of touch.”
Like the staff of Christie’s Place, TransAccess staff members recognize that to keep people connected to the program, it has to feel like a home. And what is home, asks Lin, but a place where you can be exactly who you are? Where it doesn’t matter if you “fail,” or relapse on drugs, or it takes many stops and starts for you to stay connected to HIV care? Where you can feel safe—not only physically and psychologically, but also where there’s safety from judgement around the actions you take in your own life?
“I tell trainees I can teach anyone to come up with an HIV regimen; the hard part is in that dance: How do you help a client feel safe—in the environment, and with you?”
Lin and his staff telegraph that sense of safety, in part, by working hard to follow through on their promises. “A lot of trans people have a hard time with trust, may feel let down and betrayed by families as well as providers,” Lin says. “If we say we will help you with something or do something, we do it.” Using the example of a form for a discount transit pass: It may not seem like a big deal to a provider if they forget, but it may be what’s most important to a client—and a host of negative past experiences may leave her wondering whether her provider failed to give her the form because she is trans. “With historical baggage, we have to work harder to prove trustworthiness; we do this by being very transparent.”
Another aspect of the TransAccess approach is to invite clients to be involved in their own decisions, and to make sure they have all the information to make them. “Some physicians would feel the need to get a client’s HIV in control before they start hormone therapy,” Lin explains. “A collaborative approach would mean explaining more, asking questions like: ‘Would it make a difference to you if you knew that a more successful gender transition is possible once your virus is under control? We can do it your way—how do you think that might change your feelings about being on HIV meds? If we start hormones first, would it give you a sense of hope and motivation?’”
For clients who have experienced many disparities and may feel that they have very little power, an important step for a provider is to try to level the playing field a bit. This approach is also key to the work of Christie’s Place, where informed consent is vital to a client’s sense of being a partner in her health care—of knowing her ideas, opinions and decisions matter. “In situations involving intimate partner violence or childhood abuse, there’s a power differential,” adds Falvey of Christie’s Place, pointing to the impact of trauma histories on experiences of care. “Violence can remove that aspect of human dignity.”
Even though TransAccess sees some of San Francisco’s most complex clients, the percentage of clients whose HIV has reached undetectable levels is quite high: 75 percent or more for women receiving primary care through the project. In keeping with SAMHSA’s trauma-informed guidelines, this kind of care “is not about dogged focus on a particular model; it’s about the approach—a sense of home and welcome, trust and safety; a place that can be flexible enough to meet needs.
“That’s the higher bar I would challenge all of us to hold,” he says. “It’s not just about an undetectable viral load—in many ways that’s the easiest part—but how to help somebody to not be vulnerable to the same forces that can pull them back down? How to get people off the streets? Help them find economic empowerment opportunities?”
In the long view, support for such an approach can even help save costs, according to Lin—the alternative is someone will continue to be stuck and decline until something catastrophic happens to their health.
“Trauma-informed principles are generally good for all populations,” Lin muses; “but it is all the more important to carve out time and space to really practice them well with clients most likely to drop out of care—and least likely to walk in your door in the first place.”
Vanessa Johnson (third from right) and friends at Common Threads’ Marketplace, USCA 2015.
Photo courtesy of Lepena Reid
‘A breakdown is a Hallelujah—an opportunity to cry, or feel, what you have not until then. No matter how hard it was, you overcame it, because you’re standing here.’
—Vanessa Johnson, Founder of Common Threads
Common Threads:
Healing wounds, finding voice
Storytelling is the foundation of Common Threads, a multi-stage community-based intervention that addresses barriers to care and a high quality of life: by increasing disclosure, combatting poverty by fostering economic empowerment, and preparing women with HIV to be advocates on behalf of their communities as well as themselves.
According to founder Vanessa Johnson, the intervention supports women in a healing process around their HIV diagnosis, including how earlier life experiences and even historic experiences within their families may have increased their vulnerability to HIV and/or unfavorable health outcomes. The first stage of the intervention is a three-day training where interactive discussion tools and activities are used to guide participants in thinking about their life stories in different ways, starting long before they became HIV-positive.
“The seed of shame and guilt was planted before HIV,” explains Johnson, who has herself been living with HIV since 1990. “When you get your diagnosis, whatever self-esteem issues you had get solidified.
“Before we can move on to helping women live the lives they could live, we have to deal with the initial trauma.” Once women create a space to think about themselves differently, says Johnson, they are likely to take better care of themselves.
Further, a requirement for eligibility in the highly sought-after training is that women partner with an HIV service provider or other community organization in their area to support their participation in Common Threads—so that, if the training opens a woman’s past wounds, she is already connected to a service provider to address issues that have come up. This connection to a local service provider can help deepen a woman’s engagement in care after the first phase of the training.
“Women can be very broken when they arrive at a Common Threads training; they may say something like ‘I was told by my case manager that I need to be here—my doctor is saying I need to go on meds, and I don’t want to.’ It’s powerful for them to be in the same room, sharing with other women who may already have crossed that bridge.” Another requirement is that a woman must be willing to self-disclose her HIV-positive status as part of the training.
The facilitation team consists of two peer facilitators who are women living with HIV; one group facilitator; and a licensed clinician. The clinician has two roles during the training: to educate about the myriad impacts of trauma and to support women through emotional breakthroughs, or breakdowns, over the course of the training.
“When you break down, you are getting to you,” Johnson says. “A breakdown is a ‘Hallelujah’—an opportunity to cry, or feel, what you have not until then.” Part of facilitators’ roles is validating that a woman’s trauma is not her fault. “No matter how hard it was, you overcame it, because you’re standing here.”
“Women in a room together get a lot from each other’s stories,” says Johnson. “It brings up their shared humanity.” Women recognize, perhaps for the first time, that they don’t have to bear the whole burden of shame and guilt around HIV—that in light of past history, and what may have happened to them, HIV could have happened to anybody.
In her work, Erin Falvey, of Christie’s Place, sees the ability to have a voice about what’s happening in one’s life as a trauma recovery strategy. In this way, the stories uncovered and developed as part of Common Threads can be tools for advocacy. With Common Threads as one inspiration, WHP and PWN-USA are working to develop an intervention, led and facilitated entirely by and for women living with HIV, combining trauma healing and advocacy training for participants to lift their voices and take action to make changes that affect their lives and the lives of their communities.
The goal of Common Threads in an earlier version was for women to then go out into the community to tell their stories publicly—and, when there was funding available, be paid a stipend for their work. Public storytelling is an aspect of Common Threads alumnae’s experience, but this economic aspect evolved into the Microenterprise Circle (the ME Circle), the second stage of the Common Threads program. In the ME Circle, women develop an economic collective project, learn crafting techniques, and continue to explore the impact of HIV on their personal stories and communities.
A 2014 article in the Journal of Health Disparities Research and Practice explores Common Threads as a gender-responsive vocational intervention for African American women living with HIV. As a board member of the National Working Positive Coalition and the co-owner of her own company, Ribbon Consulting Group, economic empowerment is an important theme for Johnson. However, for her, the role of the ME Circle is to maintain groups of Common Threads graduates as a collective and a mutual support system of women that could accomplish shared goals. (Read the journal article on Common Threads: digitalscholarship.unlv.edu/cgi/viewcontent.cgi?article=1250&context =jhdrp.)
“The financial piece,” as Johnson puts it, “is gravy”—and has assisted women in increasing their financial independence. The Common Threads Marketplace—the third stage of the program, in which women participate as vendors at community and conference events and sell their jewelry, pillows, poetry, and other products they’ve produced—has been a feature of the past three United States Conferences on AIDS (USCAs), in addition to numerous local and regional events; Common Threads alumnae are planning for an even more impactful presence at USCA 2016.
Common Threads is primarily geared toward women of African descent. “It’s important to have that commonality,” says Johnson. “We only have three days—we don’t have much time to explain what it means to be Black so we can move on.” In mixed groups, this part can take longer—and versions of the training module have been offered to mixed-race groups of women living with HIV. One-and-a-half-hour and one-day snapshots highlighting Common Threads tools or techniques have also been offered, to share a taste of the program in less than three days. The group then usually works to find funding to bring the full training to their area.
Since 2008, Common Threads trainings have been conducted with groups of women in about a dozen areas—including a number of locations in the U.S. South, where both poverty and HIV among African American women are especially prevalent. One barrier to making Common Threads more widely accessible is the expense. The full three-day training can cost $15-20,000 to feed and house eight to 12 women for three days, as well as pay facilitators.
“It’s an investment; if we want that desired return of trauma recovery, healing, agency, and advocacy, we need to make that investment.
“In the end it will save money, but you have to spend some,” says Johnson. “It would be helpful to be able to say that, if you sent this person to a professional counselor for a comparable experience, it would cost this much more money.”
In Johnson’s experience, transformative interventions like Common Threads can prime participants for engagement in therapy. “They can go to a counselor fertile, ready to speak, knowing what issues they need to take care of,” she says. “Peer-led interventions can be supportive of professionals in that way.”
“Our whole system is builton survival of the fittest,” Johnson comments. “We have to turn in a direction away from this, toward a trauma-informed approach—toward the reality that all humanity is valuable.”
Olivia Ford has been engaged with HIV-related media since 2007. She currently works as a freelance editor and writer, and is based in New Orleans, Louisiana.
Videos with TransAccess clients from API Wellness, community partner for the TransAccess program described above, are below:
Angel by Angel Blaylock (3:23). Angel shares some of the struggles that make it harder for her to stay in HIV treatment. She also tells us quite clearly and beautifully what *does* work: a clinic that’s a “home.” youtu.be/gG6PH23251M
Turning Point by Anuhea Talia Dela Cruz (3:09). Talia tells us how vital acceptance of her transition and gender identity is to her health—and how damaging it can be when a medical provider is not transgender-competent. youtu.be/cL12eGakrF0
In Search of Myself by Johanna Brown (3:24). Johanna tells us how embracing her gender identity has helped her deal with her HIV diagnosis. In her own words, Johanna is a strong, Black woman who now speaks out on behalf of her community. youtu.be/ZIbD9mOSgMU